Ningjian Wang et al. studied the association of nigh shift and atrial fibrillation (AF), and found that both current and lifetime night shift could lead to higher risk of AF.
Abstract
Aims
The aim of this study was to test whether current and past night shift work was associated with incident atrial fibrillation (AF) and whether this association was modified by genetic vulnerability. Its associations with coronary heart disease (CHD), stroke, and heart failure (HF) were measured as a secondary aim.
Methods and results
This cohort study included 283 657 participants in paid employment or self-employed without AF and 276 009 participants free of CHD, stroke, and HF at baseline in the UK Biobank. Current and lifetime night shift work information was obtained. Cox proportional hazard models were used. Weighted genetic risk score for AF was calculated. During a median follow-up of 10.4 years, 5777 incident AF cases were documented. From ‘day workers’, ‘shift but never/rarely night shifts’, and ‘some night shifts’ to ‘usual/permanent night shifts’, there was a significant increasing trend in the risk of incident AF (P for trend 0.013). Usual or permanent night shifts were associated with the highest risk [hazard ratio (HR) 1.16, 95% confidence interval (CI) 1.02–1.32]. Considering a person’s lifetime work schedule and compared with shift workers never working nights, participants with a duration over 10 years and an average 3–8 nights/month frequency of night shift work exposure possessed higher AF risk (HR 1.18, 95% CI 0.99–1.40 and HR 1.22, 95% CI 1.02–1.45, respectively). These associations between current and lifetime night shifts and AF were not modified by genetic predisposition to AF. Usual/permanent current night shifts, ≥10 years and 3–8 nights/month of lifetime night shifts were significantly associated with a higher risk of incident CHD (HR 1.22, 95% CI 1.11–1.35, HR 1.37, 95% CI 1.20–1.58 and HR 1.35, 95% CI 1.18–1.55, respectively). These associations in stroke and HF were not significant.
Conclusion
Both current and lifetime night shift exposures were associated with increased AF risk, regardless of genetic AF risk. Night shift exposure also increased the risk of CHD but not stroke or HF. Whether decreasing night shift work frequency and duration might represent another avenue to improve heart health during working life and beyond warrants further study.
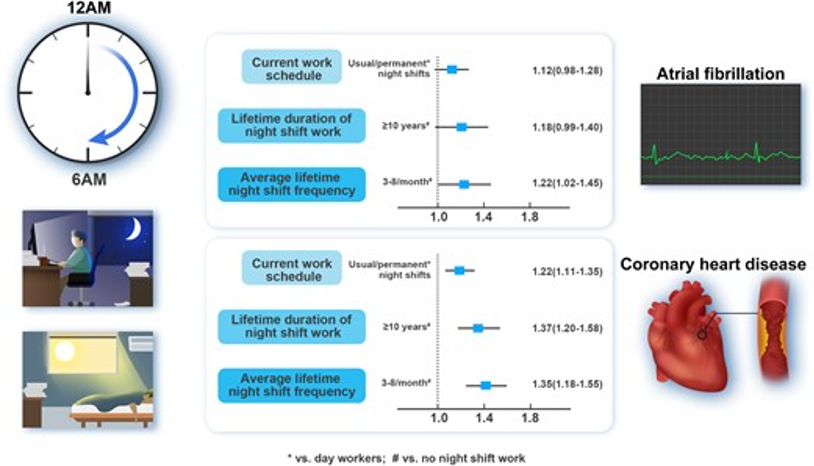
This study demonstrates that both current and lifetime night shift exposures were associated with increased risk of atrial fibrillation and coronary heart disease.
